Introduction
With more than 32 million vaccine doses administered and more than 90 per cent of people aged 12 and over fully vaccinated, the province has fared better than many jurisdictions during the COVID-19 pandemic. Ontario has made unprecedented investments that have helped the province respond effectively and decisively during a period of global instability.
Ontario’s Plan to Stay Open includes concrete measures to build Ontario’s health care workforce, shore up domestic production of critical supplies, like personal protective equipment and vaccines, and invest in hospitals, long-term care homes and home care. These measures would add nurses, doctors and personal support workers, build hospital and long-term care beds, and support seniors so they can receive care and stay in the comfort of their own homes longer.
Expanding Ontario’s Health Care Workforce
Recruiting and Retaining Health Care Providers in Underserved Communities
As part of Ontario’s commitment to building a stronger health care workforce, the government is investing $142 million, starting in 2022–23, to recruit and retain health care workers in underserved communities. This will start with $81 million, beginning in 2022–23, to expand the Community Commitment Program for Nurses for up to 1,500 nurse graduates each year to receive full tuition reimbursement in exchange for committing to practice for two years in an underserved community.
Starting in spring 2023, the government will launch the new $61 million Learn and Stay Grant. Applications will open for up to 2,500 eligible postsecondary students who enrol in priority programs, such as nursing, to work in underserved communities in the region where they studied after graduation. The program will provide upfront funding for tuition, books and other direct educational costs.
These investments build on the government’s commitment as part of the 2021 Ontario Economic Outlook and Fiscal Review: Build Ontario to invest $342 million that will add over 13,000 workers to Ontario’s health care system, including over 5,000 new and upskilled registered nurses and registered practical nurses as well as 8,000 personal support workers.
The expansion of the Community Commitment Program for Nurses and the new Ontario Learn and Stay Grant will support the attraction and retention of skilled health care professionals in rural and Northern Ontario and ensure better access to quality health care services in rural and remote communities.
Robin Jones
Mayor, Village of Westport
Chair, Rural Ontario Municipal Association (ROMA)
The government also proposes to make it easier and quicker for foreign-credentialled health workers to begin practising in Ontario by reducing barriers to registering with and being recognized by health regulatory colleges. Proposed legislation would prohibit regulatory colleges from requiring Canadian work experience as a qualification for registration, subject to any exemptions provided for in accompanying regulations. Proposed legislative amendments would also require regulatory colleges to certify potential applicants in a timely manner so that internationally trained health care workers can start work as soon as possible.
Supporting Retention of Nurses
Retaining and hiring more nurses is another strategy Ontario is using to strengthen the health care workforce. The government is investing $764 million over two years to provide Ontario’s nurses with a lump sum retention incentive of up to $5,000 per person. This funding will help to retain nurses across the health sector and stabilize the current nursing workforce to provide patients with access to the health care they need and deserve. Nurses eligible to receive the payment include nurses in hospitals, long-term care and retirement homes, home and community care, primary care, mental health and addictions, emergency services, corrections, and a range of other community-based and developmental services including youth justice. Nurses in a management or supervisory role who were redeployed to a direct patient care role also qualify.
Modernizing Clinical Education for Nurses
To address the shortage of health care professionals in Ontario, the government is investing $124.2 million over three years starting in 2022–23 to modernize clinical education for nurses. This investment will enable publicly assisted colleges and universities to expand laboratory capacity supports and hands-on learning for students, providing opportunities for learners to demonstrate their skills in practical settings.
Permanently Enhancing the Wages of Personal Support Workers
Since October 1, 2020, the government has invested more than $1.3 billion to provide a temporary wage enhancement to more than 158,000 personal support workers (PSWs) and direct support workers (DSWs) providing publicly funded services in hospitals, long-term care, home and community care and social services.
The government is working to fulfil its commitment to introduce a permanent PSW and DSW wage enhancement by investing approximately $2.8 billion over the next three years to make the current temporary program permanent. The permanent wage enhancement will help to continue these important supports in the long-term recovery from the pandemic and to build a stronger and more resilient health care system that is better prepared to respond to crisis.
Expanding Medical Education, including to Brampton and Scarborough
To strengthen Ontario’s health care system across the province, the government is investing $42.5 million over two years beginning in 2023–24 to support the expansion of undergraduate and postgraduate medical education and training in Ontario. This expansion will result in an increase of 160 undergraduate seats and 295 postgraduate positions over the next five years.
All medical schools across Ontario will benefit from this expansion, including the Queen’s University School of Medicine, the Northern Ontario School of Medicine, the new University of Toronto’s Scarborough Academy of Medicine and Integrated Health, and the Ryerson School of Medicine in Brampton when it becomes operational. These investments will help recruit future health care workers and support improved care for underserved areas of the province.
Increasing the number of doctors, nurses and personal support workers in Ontario is a key element of the government’s Plan to Stay Open. This requires recruitment and retention of nurses and personal support workers, and investing in the students of today who will become the skilled health care professionals of tomorrow. Expanding medical education will result in more doctors serving in Ontario and better access and quality of care for hard-working families across the province.
Expanding the Health Sector Workforce
Ontario’s dedicated health care workers are the foundation of the province’s health care system. To build on the 8,600 health care workers who joined the system since March 2020, Ontario is accelerating its efforts to expand hospital capacity and build up the province’s health care workforce to help patients access the health care they need when they need it. This is why Ontario is investing $230 million in 2022–23 to enhance health care capacity including critical care in hospitals. This includes:
- Deploying over 3,300 and hiring more than 1,700 additional health care students in hospitals;
- Supporting over 150 and hiring more than 220 additional nursing preceptors and coordinators to support health care students;
- Redeploying over 350 hospital support aides;
- Supporting up to 1,000 internationally educated nurses to become accredited nurses in Ontario through the Supervised Practice Experience Partnership program; and
- Providing up to 400,000 hours of additional service delivery by redeployed medical residents to support critical care capacity.
Ontario is also investing $49 million over three years to develop new programs to train, recruit and retain critical care workers. These programs will help hospitals meet growing needs by:
- Supporting Intensive Care Unit (ICU) staff across 74 hospitals to address increased demand for services;
- Training 540 interns for both respiratory therapist and registered nurse positions; and
- Funding more than 10 innovative projects to increase ICU nurse retention.
These investments build on the government’s commitment as part of the 2021 Ontario Economic Outlook and Fiscal Review: Build Ontario to invest $342 million over the next five years to increase health human resources through recruitment initiatives.
Shoring Up Domestic Production of Critical Supplies and Ensuring Ontario is Prepared for Future Emergencies
Increasing Ontario Made Personal Protective Equipment
The COVID-19 pandemic revealed challenges in securing Critical Supplies and Equipment (CSE), such as Personal Protective Equipment (PPE), to safeguard the people of Ontario, including frontline workers and vulnerable persons. Since the onset of the pandemic, Ontario has been procuring these supplies and equipment through its traditional suppliers as well as working directly with manufacturers.
By promoting and supporting Ontario manufacturing and innovation, the province is now producing a wide variety of PPE and CSE right here in Ontario. Over 92 per cent of the government’s forecasted PPE spend for the next 18 months will come from Ontario or Canadian sources. This includes the production of N95 respirators at a newly expanded 3M facility in Brockville, as well as sourcing 200 million Level 1 and Level 2 surgical/protective masks annually for five years through four Ontario-based companies — PRIMED Medical Products, CANADAMASQ, Viva Healthcare Packaging Canada and JY Care. In addition, the government continues to leverage the province’s extensive manufacturing capability wherever possible to maintain a stockpile of quality PPE and CSE, which could strengthen PPE and CSE supply chains.
To ensure the province will no longer have to rely on foreign markets to acquire PPE, as well as to reduce supply chain vulnerability, Ontario also plans to support the domestic production of nitrile gloves. This is part of Ontario’s supply chain strategy, led by Supply Ontario, to continue to protect the health and safety of the people of Ontario and build strategic domestic production and supply chain capacity for critical goods and services.
As part of the Pandemic and Emergency Preparedness Act, 2022, Ontario will prohibit any person from selling any personal protective equipment or critical supplies supplied free of charge by the government. This will help ensure that those who take advantage of hard-working people who play by the rules will face stiff penalties for their actions.
Supporting Safety and Security through the Ontario Together Fund
In April 2020, Ontario launched the $50 million Ontario Together Fund to help manufacturers provide innovative solutions or retool their operations in order to manufacture PPE and essential medical supplies. In March 2021, Ontario announced an additional $50 million investment to continue supporting local businesses for the safety and security of the people of Ontario.
As of early April 2022, more than $77 million of the Ontario Together Fund’s support has been committed, leveraging almost $230 million in investments in building Ontario’s domestic capacity to manufacture PPE and provide other solutions in response to COVID-19 in order to help build resilience in the health care sector. Examples of recent investments made through the fund include:
- In April 2022, an investment of more than $3.7 million by Toronto Research Chemicals, supported by $2.5 million through the Ontario Together Fund. The Toronto company will be developing a line of chemicals used in the development of polymerase chain reaction test kits, including those used for COVID-19 detection.
- In January 2022, an investment of more than $37 million by Kawartha Ethanol Inc., supported by $2.5 million through the Ontario Together Fund. The new investment will help the Havelock-based company expand its local production capabilities to manufacture high-grade, pure ethanol for hand sanitizers and disinfectants.
Strengthening Reporting and Accountability for Personal Protective Equipment
Since March 2020, the people of Ontario have taken steps to protect their families, friends and neighbours. They made sacrifices based on a promise that they would one day see a return to the hard-earned freedoms and opportunities that make Ontario a place of limitless possibility. This is why the government will ensure that lessons learned during the past two years inform how the government prepares for emergencies. Global shortages at the beginning of the pandemic showed that Ontario needs a reliable, robust, centralized PPE and CSE supply chain to meet the needs of frontline workers and the people of Ontario.
As part of Ontario’s Plan to Stay Open, the province will be required to maintain a PPE and CSE stockpile to meet needs during both normal operations and extraordinary events. The plan sets out key requirements for planning, procurement, storage, distribution and management of PPE and CSE. By making these changes, the people of Ontario can have confidence that the government is protecting Ontario with a stable and steady supply of equipment in both good times and in bad.
Building a Robust Life Sciences Sector
The COVID-19 pandemic has highlighted the importance of having a strong domestic life sciences sector. Innovations from the sector also have incredible therapeutic and commercial potential. This includes the development and manufacturing of health care solutions like vaccines, regenerative medicines, as well as advanced therapies.
The government has launched a new life sciences strategy — Taking Life Sciences to the Next Level — which is the first of its kind in over a decade. The strategy outlines the government’s plan to build up and help grow the sector and secure new investments in next-generation health technologies, medicines and vaccine manufacturing. It also sets out an ambitious goal to grow Ontario’s biomanufacturing and life sciences sector employment to 85,000 workers in high-value jobs by 2030, a 25 per centincrease from 2020.
To support the new strategy, the government will invest $15 million over three years in a new Life Sciences Innovation Program. This program will help Ontario’s small and medium-sized enterprises in the life sciences sector develop and scale up the commercial potential of therapeutics and medical and digital technologies, such as cell therapies, mRNA vaccines and applications of artificial intelligence to improve diagnosis and treatment of disease.
Preparing for Future Emergencies
To support a coordinated, whole-of-government approach, the Pandemic and Emergency Preparedness Act, 2022 will require that the government monitor provincial hazards and risks and provide information to the public. The government will be required to have a provincial emergency plan that includes a mandatory review and update at least every five years. These changes will help ensure the government is ready to respond to any future emergency or pandemic.
The government is also committing an additional $3.5 million in 2022–23 to improve emergency readiness and protect the people of Ontario in the event of major emergencies. This funding will enhance the government’s coordinated approach to emergency management through additional capacity to plan, prepare, respond and recover from emergencies.
Building More Hospital Beds and Improving Patient Care
Building and Improving Hospitals
Ontario is committed to building a health care system that puts patients first. This is why the government is investing more than $40 billion over the next 10 years in hospital infrastructure, including about $27 billion in capital grants, to create more capacity and address long-standing bed shortages. This is $10 billion more for hospital and health care centre infrastructure than the commitment in the 2021 Budget. These investments will improve and increase space in hospitals and community health centres and build new health care facilities.
As part of its plan to build a stronger, more resilient health care system that is better prepared to respond to crisis, the Ontario government is implementing the most ambitious plan for hospital expansion in Ontario’s history. This includes supporting more than 50 major hospital projects that would add 3,000 new beds over 10 years.
Additional investments will support the continuation of over 3,000 acute and post-acute beds in hospitals and alternate health care facilities, as well as hundreds of new adult, pediatric and neonatal critical care beds.
The government’s record investments in hospital renewal and expansion will address the increasing need for health care services in growing communities and provide essential care to patients and their families across the province. This includes planning for critical hospital expansions at:
- William Osler Health System – Brampton Civic Hospital to increase cancer treatment capacity in Peel Region making it easier to access high-quality cancer treatment closer to home;
- Grand River Hospital and St. Mary’s General Hospital Joint Redevelopment Project to build a new joint acute care facility and expand existing facilities in the Kitchener-Waterloo region;
- Southlake Regional Health Centre – Phased Redevelopment Project to build a new acute care hospital and expand the existing Newmarket site to accommodate ambulatory care services;
- Sunnybrook Health Sciences Centre Bayview Campus to build a new critical care and complex malignant hematology tower to add new ICU beds and modernize surgical inpatient units;
- The Royal Victoria Regional Health Centre – Phased Redevelopment Project to build a new facility at the South Campus in Innisfil with an ambulatory care centre and urgent care services; and
- Brant Community Healthcare System facilities in Paris and Brantford to increase bed capacity in Southwestern Ontario and accommodate new inpatient and intensive care units.
Communities in Collingwood, Kingston and Moosonee will soon have access to new, state-of-the-art health care facilities to provide high-quality care to the people of these regions. Other critical investments in hospital projects proceeding to construction include:
- Oak Valley Health – Uxbridge Hospital Redevelopment project to replace the current aging facility, expand specialized outpatient clinics and create a community health hub with nearby long-term care services;
- Stevenson Memorial Hospital – Phase 1 Redevelopment project to renovate the existing site to increase bed complements and modernize emergency, diagnostic and surgical services;
- Lakeridge Health – Bowmanville Redevelopment project to renew infrastructure and renovate the existing facility to accommodate a new Neonatal Intensive Care Unit and expand acute inpatient care, emergency, critical care and rehabilitation services;
- Muskoka Algonquin Healthcare – Hospital Redevelopment project to redevelop acute care hospitals in Huntsville and Bracebridge to improve community services and access to diagnostic imaging; and
- Wallaceburg Sydenham Hospital, part of the Chatham-Kent Health Alliance – Capital Redevelopment project to build new emergency, laboratory and diagnostic departments.
Table 1.4
Projects Supporting Stronger, More Resilient Health Care
Northern
- Thunder Bay Regional Health Sciences Centre – Cardiovascular Surgery Program – New investment to bring cardiac care closer to home and enable future expansion of dialysis services.
- Weeneebayko Area Health Authority – Health Campus of Care – New culturally appropriate health campus that will include a new hospital and a lodge in Moosonee, as well as a new ambulatory care centre on Moose Factory Island.
- Muskoka Algonquin Healthcare – Hospital Redevelopment Project – Redevelopment of acute care hospitals in Huntsville and Bracebridge to improve community services and access to diagnostic imaging.
- Centre de Santé Communautaire de Timmins – Building a new Francophone community health centre to consolidate primary care, nursing, and mental health and addictions services in one modern facility.
Eastern
- Kingston Health Sciences Centre – Redevelopment Project – Redevelopment of the Kingston General Hospital and regional trauma centre to accommodate inpatient, surgical and emergency department growth.
- Quinte Health Care – Prince Edward County Memorial Hospital Redevelopment Project – Replacement of the existing hospital on the Picton site with a new facility to meet increasing demand for health services in the area.
- Carlington Community Health Centre – Expansion Project – Renovations to existing facility and fit-up of adjacent new facility to expand the centre’s services and create a community health hub in Ottawa.
- The Ottawa Hospital – Civic Campus Redevelopment Project – Redevelopment of the existing hospital and regional trauma centre on a new site to expand access, replace aging infrastructure and meet capacity needs.
Southwestern
- Canadian Mental Health Association (CMHA) Middlesex Mental Health and Addictions Crisis Centre Project – Renovations to create a new 10-bed mental health crisis centre to divert patients from acute care hospital emergency departments and to provide more appropriate community care for people in crisis.
- Wallaceburg Sydenham Hospital, part of Chatham-Kent Health Alliance – Capital Redevelopment Project – Construction of a new emergency department as well as new diagnostic imaging and laboratory departments to modernize services.
- West Lincoln Memorial Hospital Redevelopment Project – A new hospital building on the existing site with emergency care, inpatient, maternal and newborn services and day surgery.
- South Bruce Grey Health Centre – Kincardine Site Phase 1 Redevelopment Project – Expansion of the diagnostic imaging department to add a new computed tomography scanner to bring care closer to home.
- Windsor Regional Hospital – New Windsor-Essex Acute Care Hospital – Support for a new hospital to consolidate acute care services, while retaining the existing Ouellette site for urgent care and ambulatory services.
Central
- Oak Valley Health – Uxbridge Hospital – Redevelopment – Building a new, modern hospital on the existing Uxbridge site to replace the current aged building, expand specialized outpatient clinics and create a community health hub.
- Southlake Regional Health Centre: Redevelopment – Planning for redevelopment to add new beds and expand surgical capacity and inpatient mental health care.
- William Osler Health System – Radiation Oncology Project – Support to plan for new ambulatory outpatient cancer services at the Brampton Civic Hospital site.
- North York General Hospital Phase I Redevelopment – Construction of a new inpatient care tower and renovations at the North York General Hospital site to address projected growth in acute care programs.
- Stevenson Memorial Hospital – Phase 1 Redevelopment – Renovations to the existing site to increase beds and modernize emergency, surgical, and diagnostic services, as well as the birthing suite.
- Unity Health Toronto – St. Joseph’s Health Centre – Major Redevelopment Project – Construction of a new clinical services tower and expansions to the medical and surgical inpatient programs to expand integrated health care services and reduce wait times.
Source: Ontario Ministry of Health.
Building More Hospital Beds
Making Historic Investments in Hospitals
While hospitals faced many challenges even before the pandemic, COVID‐19 stretched them to the limit. The government continues to ensure its health care system is prepared to respond to any crisis and protect the health and well‐being of the people of Ontario. This is why Ontario is investing an additional $3.3 billion in 2022–23, bringing the total additional investment in hospitals to $8.8 billion since 2018–19. Funding in 2022–23 includes:
- $1.5 billion to support the continuation of over 3,000 acute and post-acute beds, and hundreds of new adult, pediatric and neonatal critical care beds;
- $827 million representing a four per centincrease from the previous year to ensure public hospitals are able to meet patients’ needs and increase access to high-quality care;
- $300 million to address surgical and diagnostic imaging recovery; and
- $250 million to support health human resources.
This is a historic investment that will provide the people of Ontario with access to the high quality of care that they deserve. The government is now in a place where it can use the lessons learned over the past two years and take actions to ensure Ontario’s health system is even better, stronger and more resilient in the face of any future challenge.
Maintaining Additional Hospital Beds

Ontario has built unprecedented hospital capacity since the start of the COVID-19 pandemic, creating more than 3,000 acute and post-acute hospital beds across the province — equivalent to six large community hospitals. Ontario is investing $3.5 billion over three years starting in 2022–23 to support the continuation of over 3,000 hospitals beds put in place during the pandemic. This will increase hospital capacity, reduce potential future occupancy pressures and end hallway health care.
Expanding Critical Care Capacity
Since the outset of the pandemic, the government has added hundreds of critical care beds. Providing the necessary intensive care unit capacity is critical to treating the people of Ontario with the greatest need. This is why Ontario is investing $1.1 billion over three years to support the continuation of hundreds of new adult, pediatric and neonatal critical care beds in the province. This investment will ensure hospital beds are available for patients in need of urgent care.
Increasing Access to High-Quality Care
The government is also investing an additional $2.5 billion over three years to support key health care needs in Ontario hospitals, including:
- Supporting Demand and Patient Growth: Supporting all publicly funded hospitals, including specialty psychiatric hospitals, specialty children’s hospitals and small hospitals, to keep pace with patient needs and to increase access to high-quality care for patients and families across Ontario;
- Providing Priority Services: Supporting an aging population and growing need for key procedures and programs including cardiac care, cataract procedures, knee and hip replacements and critical care services; and
- Expanding Hospital Facilities: Investing in hospital operations including clinical services and facility costs.
Building Surgical Capacity
Addressing Surgical Recovery in Hospitals
To increase capacity and to build a strong and resilient health care system, the government is investing $300 million in 2022–23 as part of the province’s Surgical Recovery Strategy, bringing the total investment to roughly $880 million since the start of the pandemic.
The Surgical Recovery Strategy will increase scheduled surgeries, procedures and appropriate diagnostic imaging services with a focus on areas with the greatest reduction in services due to the pandemic. This strategy will also provide funding to hospitals for innovative solutions to address local needs and increase surgeries across the province. This investment will also support over 150,000 additional hours of MRI and CT diagnostic imaging scans.
Making Historic Investments in Long-Term Care
The Ontario government is making swift progress in fixing the long-term care sector and helping Ontario’s seniors get the quality of care and quality of life they deserve. A key pillar of this plan is to build modern, safe and comfortable homes for seniors, so that a long-term care bed is available for loved ones when it is needed.
Ontario now has over 31,000 new and over 28,000 upgraded beds in the development pipeline — and is on track to build more than 30,000 net new beds across the province by 2028. These beds are supported by planned investments that total a historic $6.4 billion since spring 2019. Many of these new long-term care beds will be in homes that will offer culturally and linguistically appropriate services to better serve Ontario’s seniors.
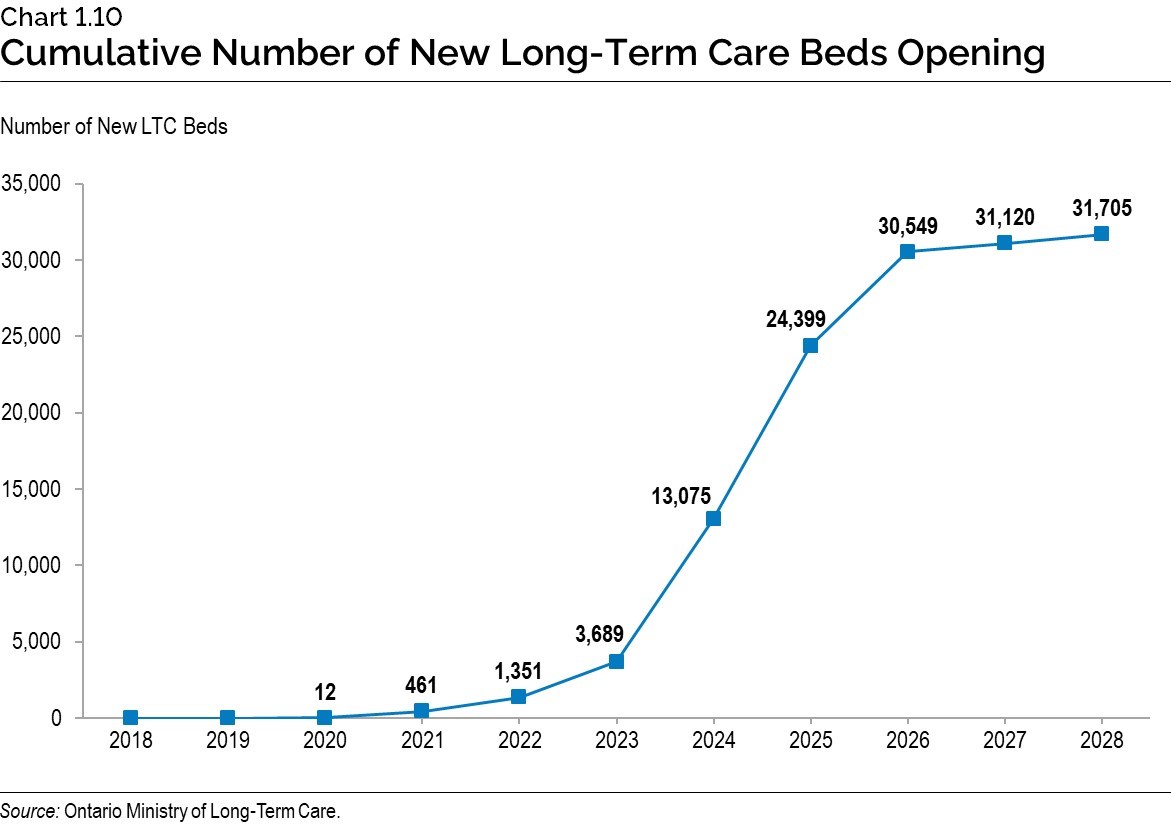
Table 1.5
Long-Term Care Projects Highlights
Planning
- Schlegel Villages will build 640 new long-term care beds in Oakville using government surplus lands.
- The Northern Heights Care Community project will build 12 new long-term care beds and upgrade 148 long-term care beds in North Bay.
- The Golden Manor project will build 15 new long-term care beds and upgrade 177 long-term care beds in Timmins.
- The St. Joseph’s Health Centre Guelph expansion project will build 160 new long-term care beds in Guelph.
Under Construction
- Construction is underway for the Temiskaming Lodge project to build 46 new long-term care beds and upgrade 82 long-term care beds in Temiskaming Shores.
- Construction is underway for the Extendicare Sudbury project to upgrade 256 long-term care beds.
- Construction is underway for the Runnymede Long-Term Care Home to build 200 new long-term care beds in Toronto.
- Construction is underway for the Stoneridge Manor project to build 68 new long-term care beds and upgrade 60 long-term care beds in Carleton Place.
- Construction is underway for the Golden Plough Lodge Redevelopment project to build 29 new long-term care beds and upgrade 151 long-term care beds in Cobourg.
- Construction is underway for the Ritz Lutheran Villa project to upgrade 128 long-term care beds in Mitchell.
- Construction is underway for the Linhaven Long-Term Care Home project to build 13 new long-term care beds and upgrade 226 long-term care beds in St. Catharines.
- Construction is underway for the Gilmore Lodge project to upgrade 160 long-term care beds in Fort Erie.
Completed
- Lakeridge Gardens opened in March 2022 with 320 new long-term care beds in Ajax.
- The Algonquin Nursing Home project opened in June 2019 with 72 upgraded long-term care beds in Mattawa.
- Glen Hill Terrace opened in May 2021 with 160 upgraded long-term care beds in Whitby.
- The Grove Nursing Home opened in October 2021 with 36 new long-term care beds and 60 upgraded long-term care beds in Arnprior.
- The Mon Sheong Stouffville Long-Term Care Centre opened in October 2021 with 320 new long-term care beds in Whitchurch-Stouffville.
- The Villa Care Centre opened in March 2022 with 51 new long-term care beds and 109 upgraded long-term care beds in Midland.
- The Faith Manor project opened in July 2021 with 40 new long-term care beds and 120 upgraded long-term care beds in Brampton.
- The Royal Rose Place expansion opened in March 2022 with 64 new long-term care beds in Welland.
- Elmwood Place opened in September 2021 with 50 new long-term care beds and 78 upgraded long-term care beds in London.
Source: Ontario Ministry of Long-Term Care.
Adding More Specialized Long-Term Care Beds and Services
Some patients require increased levels of care and support. This is why the government is investing an additional $8.3 million over three years to add 40 Behavioural Specialized Unit beds at long-term care homes in Ajax and Mississauga. This builds on the 2019 commitment to add up to 144 additional beds, on top of the 181 Behavioural Specialized Unit beds currently available to seniors across the province.
These specialized beds help residents waiting for long-term care to receive timely access to more intensive high-quality care from nurse practitioners, registered nurses, registered practical nurses and personal support workers. Behavioural Specialized Units reduce transfers to hospital emergency departments and provide transitional and dedicated care to residents with specialized needs.
This investment reduces capacity pressures in hospitals by helping patients move from hospitals to long-term care homes more quickly. The government continues to ensure that loved ones in long-term care have access to the care they need in the most appropriate setting.
Ensuring the Voices of Long-Term Care Home Residents Are Heard
Ontario’s seniors deserve high-quality care. Ontario is making strides towards better meeting the needs of long-term care residents by hearing directly from them.
In the past, long-term care homes have used different and varied survey tools to assess a resident’s experience. This has led to the inability to compare results effectively across long-term care homes to drive consistent improvements based on residents’ experience.
The introduction of a consistent survey across the province will support a comparison across homes to inform ongoing improvements and promote transparency. The information gained from these surveys will strengthen the collective voice of residents and their family members to help ensure their needs are met.
Expanding Home and Community Care
People, including seniors, should have the option to stay in their homes and receive the care they need if they choose and if it is possible.
Home and community care keeps people healthy and at home, where they want to be, and plays an important role in the lives of more than 700,000 families annually. A strong home and community care sector is key to the government’s plan to end hallway health care and build a connected, patient-centred health care system. As Ontario continues its recovery, home and community care will play a vital role to enable seniors and others needing assistance to live independently in the community.
Additional Investments to Support Home Care
Ontario seniors and recovering patients deserve to have the opportunity to stay in the homes that they love, where they are the most comfortable. Home care supports prevent unnecessary hospital and long-term care admissions and shorten hospital stays.
The government plans to invest up to an additional $1 billion over the next three years to expand home care, improve quality of care, keeping the people of Ontario in the homes that they love, longer. The additional funding is intended to support home care providers, address rising costs and support recruitment and training as well as expand services. This investment builds on the 2021 Ontario Economic Outlook and Fiscal Review: Build Ontario investment of $548.5 million over three years to expand home care services.
With these types of investments and other developments, such as virtual care options, care at home can become a choice that seniors, recovering patients and their families make instead of only relying on more traditional venues of care.
Helping Seniors Stay in the Homes They Love
The government introduced the Ontario Seniors’ Home Safety Tax Credit for 2021 and 2022 to help seniors who want to stay in the homes they love, surrounded by the friends and families they cherish. The credit, worth 25 per cent of up to $10,000 in eligible expenses, helps cover the costs of handrails, stair lifts and other modifications to make homes safer for seniors. The maximum credit is $2,500 for each year. The credit will provide an estimated $65 million in support over 2021 and 2022. It is expected to support about 32,000 people in 2022.
Expanding Access to Community Care

Ontario is investing nearly $100 million in additional funding over the next three years to expand community care programs such as adult day programs, meal services, transportation, assisted living services and caregiver supports. This investment will also stabilize and enhance sustainability for community services to support the well-being and independence of over 600,000 people in Ontario.
Expanding Community Paramedicine for Long-Term Care across Ontario
The government is investing more than $60 million over two years, starting in 2022–23, to continue expanding the Community Paramedicine for Long-Term Care program to the 22 remaining communities and regions across Ontario. The program initially launched in five communities in April 2020 and has since been expanded to 33 communities and regions across the province. This means that more seniors across Ontario will get the care they need.
This program leverages the skills of community paramedics to provide additional care for seniors in the comfort of their own homes through:
- Access to health services 24 hours a day, seven days a week, through in-home and remote methods, such as online or virtual supports;
- Non-emergency home visits and in-home testing procedures;
- Ongoing monitoring of changing or escalating conditions to prevent or reduce emergency incidents;
- Additional education about healthy living and managing chronic diseases; and
- Connections for participants and their families to home care and community supports.
Through the Community Paramedicine for Long-Term Care program, Ontario continues to collaborate with health system partners to provide innovative services, address hallway health care and modernize the long-term care system.
Increasing Investments for Ontario’s Dementia Strategy
To support individuals with dementia and their caregivers, the government is investing an additional $5 million a year for three years. This brings total investment to $120 million over the next three years for dementia services across the province. This funding will support an additional 6,500 people in Ontario each year to live independently within their homes and to be engaged in their community.
Building Mental Health Capacity
COVID-19 has impacted the mental health of people of Ontario from all walks of life and underscores the need for a long-term plan to respond to the pandemic.
Now more than ever, it is critical to provide mental health supports to those who need it most. A strong mental health system can also help prevent those struggling with their mental health from reaching a crisis point and helps ensure patients can access support when and where they need it.
This is why the government is investing an additional $204 million to build on investments and achievements to date, and to continue to move forward with expanding existing services, implementing innovative solutions and improving access to mental health and addiction services. This investment builds on the 2020 Roadmap to Wellness, a provincial strategy to address long-standing mental health and addictions needs, with a historic investment of $3.8 billion over 10 years.
These investments are filling critical gaps and enhancing services in a range of areas, including online cognitive behavioural therapy support, child and youth mental health, addictions services, supportive housing, mental health, justice and Indigenous mental health and addictions.
Chart Descriptions
Chart 1.10: Cumulative Number of New Long-Term Care Beds Opening
Long Description: The chart shows the cumulative number of new long-term care beds opening by year, starting in 2018 and up to 2028.
2018: 0 new beds opening.
2019: 0 new beds opening.
2020: 12 new beds opening.
2021: 461 new beds opening.
2022: 1,351 new beds opening.
2023: 3,689 new beds opening.
2024: 13,075 new beds opening.
2025: 24,399 new beds opening.
2026: 30,549 new beds opening.
2027: 31,120 new beds opening.
2028: 31,705 new beds opening.
Source: Ontario Ministry of Long-Term Care.